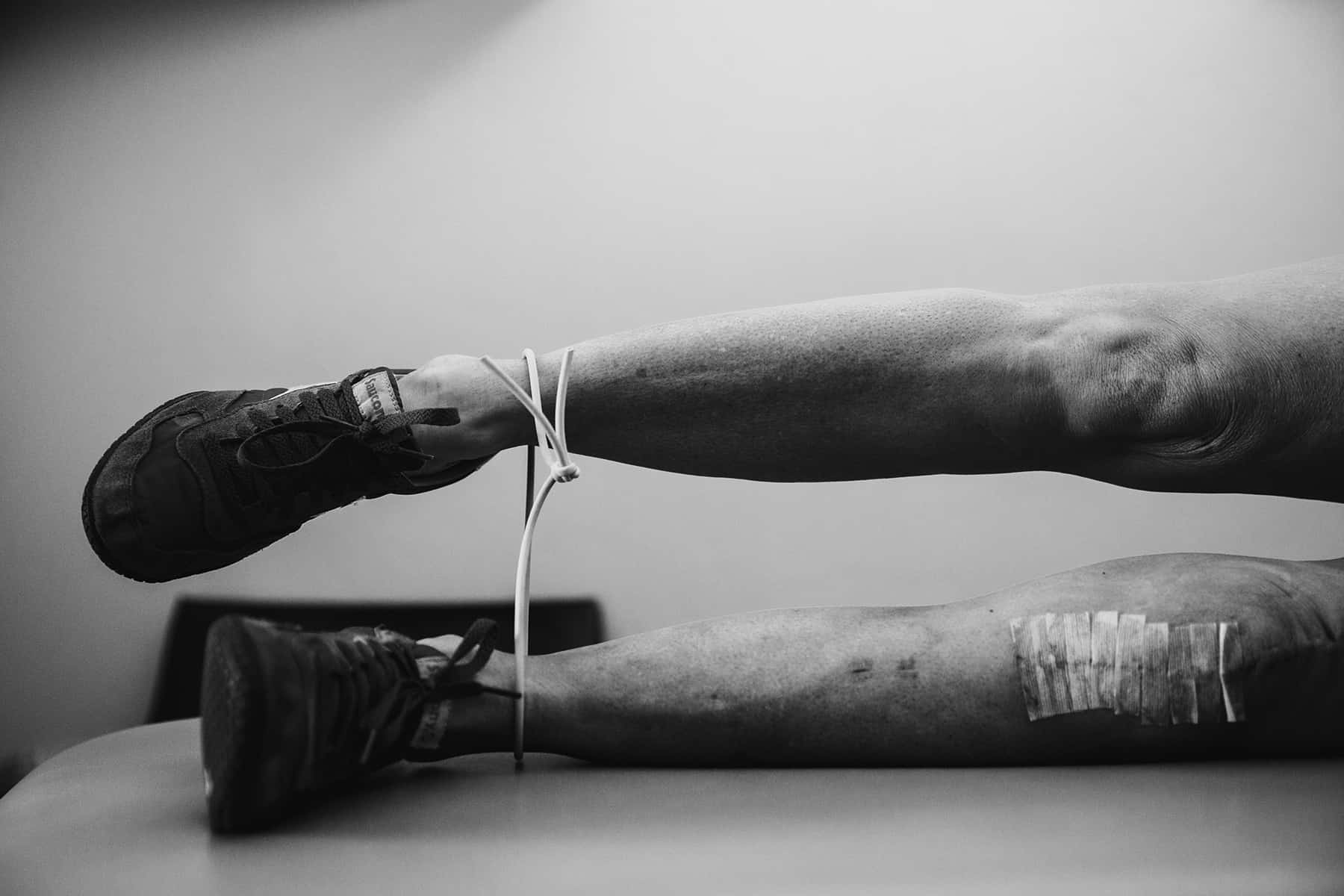
By Christina Shepherd McGuire // Photography by Shannon Corsi
—
It began with a high school tumbling accident. At camp one summer, I landed a roundoff back handspring with one foot planted firmly on the seam between the grass and the concrete sidewalk. With a twist of the ankle, my knee gave out and I heard that infamous pop. What followed was a half-baked recovery in which I continued to compete on the loose knee until it was apparent something was really wrong. I went to the doctor and was admitted for what now seems like an antiquated surgery, complete with a primitive ACL (anterior cruciate ligament) repair and meniscus removal.
Fast forward 15 years—after summiting mountaintops and skiing and snowboarding all over North America—and my compromised knee was in shambles. An MRI and subsequent “clean-out” confirmed, as suspected, I had been bone-on-bone for quite a while and early-onset osteoarthritis had set in. Still, I healed from this second surgery and went right back at it, to the tune of tearing my other ACL and succumbing to several steroidal and non-steroidal injections in my old injury site. I religiously practiced yoga, in an attempt to stay limber and mitigate the discomfort, and received acupuncture on the regular, all while knowing that, someday, I would be a candidate for one of those newfangled robotic knees.
The day finally came last winter when, 30 years after my original injury and at age 48, I could no longer ride my snowboard for more than a few smooth, powdery runs; my knee swelled while doing daily tasks like the dishes, and I couldn’t walk across the soccer field to give my kid a water bottle without limping in pain. One of my orthopedic doctors once told me: “You know you’re ready when, 1. The pain keeps you up at night, 2. You can no longer engage in the activities you love, and 3. The swelling is chronic.” I was at the point where I checked all three boxes. So, after visiting with Dr. Kevin Lee, orthopedic surgeon and sports medicine specialist at Upper Valley Orthopedics in Rexburg, receiving my x-ray results, thoroughly researching all the procedures and possible outcomes of a total knee arthroplasty, I signed myself up for a robotic-assisted surgery last February.

Christina uses a wedge to stretch her calf and regain knee extension. 
A compression-ice machine is the key to post-op pain mitigation.
Wait—48 is the new 65?
Now, when you think about joint replacements, most people immediately picture elderly individuals—often sporting a cane—who are in chronic pain and have a whole host of other medical conditions. How could I, at age 48, have x-rays that revealed the knee of a 75-year-old, advanced arthritis, bone spurs, and all?
According to William Andrew Lighthart M.D., orthopedic surgeon and hip and knee specialist at Teton Orthopaedics in Jackson, “When we talk about [joint replacements] at national meetings, the average age of hips and knees keeps inching lower.” He attributes this to the fact that surgeries are more reliable and people are less willing to put up with a bad hip or knee, noting that most patients considering the procedure are suffering from post-traumatic arthritis due to a prior ACL or meniscus tear.
Dr. Lee concurs, especially when considering the demographic in our region. “People have a high level of activity [in our area],” he says. “They don’t want to slow down and they are not willing to sacrifice activity because they have a sore knee. So, if something can restore their level of activity, they go for it, even though there is some risk.”
Dr. Lighthart mentions that, technically, knee replacements are only FDA approved for people over the age of 65, those who weigh 180 pounds or less, and those not suffering from autoimmune conditions, like inflammatory (rheumatoid) arthritis. While these recommendations have not been revised since the 1970s, even with advances in both the surgical procedures and prosthesis technology, he says that 50 percent of the surgeries he performs are “off label.”
I certainly fell into this category.

Put the Pre- Before the Re[Hab]
In the month preceding my surgery, I started a rigorous pre-hab program. I attended a weekly hot yoga class, rode my stationary bike like it was my job, and performed exercises that my physical therapist, Mike Bleffert, of Eagle Orthopedic and Sports Physical Therapy in Driggs, lined me out on. For me, the concentration was less about “getting strong” (I was already there) and more about range of motion, as my injured knee’s flexion had been compromised ever since my original surgery in 1989.
Bleffert praises the merits of pre-habilitation. “Clinically, I feel like when we get people in before surgery to work on range of motion and introduce exercises, then, after surgery, they are familiar with what they have to do,” he says. “Also, it allows us to form a relationship with the patient [before surgery], so they develop a sense of trust in us.”
My surgery day came on February 1, 2021.
“It was worse than we thought,” said Dr. Lee, as he sat at my bedside post-op. “You had no ACL left, only 50 percent of a frayed PCL [posterior cruciate ligament], and some of the worst bone spurs I’ve seen.”
I left the hospital with a level of pain that—even after experiencing all of my surgeries and delivering two children naturally—I had not yet faced in my life. I slept on the couch hooked up to my ice machine round-the-clock, blood pressure plummeting every time I took a pain pill. And I cried nearly every day for a month, wondering what I signed myself up for. Time stood still, as I abandoned my role as mother and wife to concentrate on healing.
My doctor confirmed the validity of my post-operative pain threshold. “Younger people tend to have a more acute pain sensation,” says Dr. Lee. “Older people definitely have an internal modulation system where the dial is turned down. So, while an older patient’s health may not be as good, their pain may be less severe.”
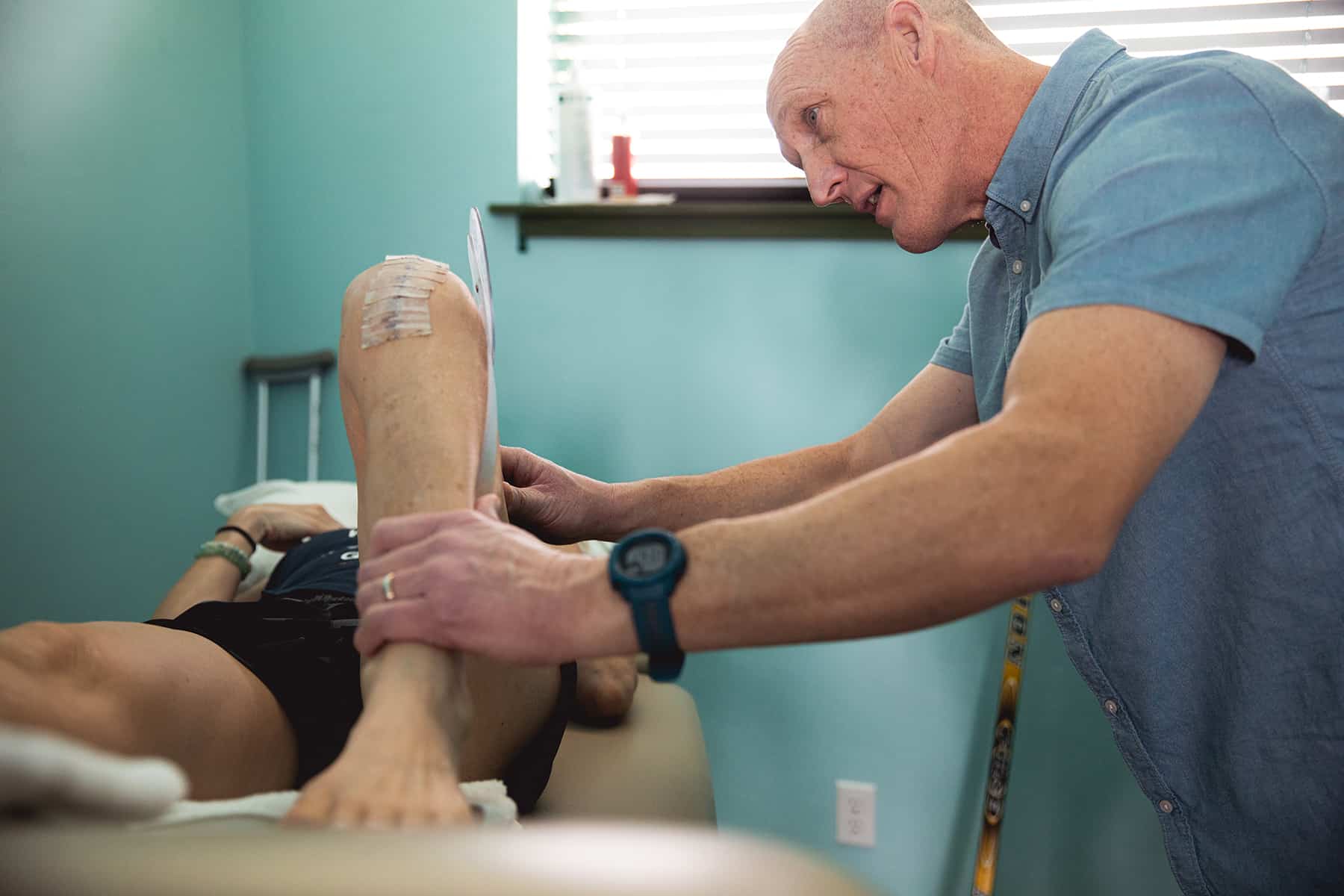
For the weeks following, Mike and I worked diligently to break down scar tissue, in an effort and regain as much knee flexion as possible. This often involved soft tissue manipulation, with a butter knife-like tool, as well as a whole host of range-of-motion exercises, like heel slides and, later, hamstring curls. Every day, despite the pain, I would wake up and do a gentle, floor-based yoga routine to stretch my hamstrings and my hips and to ease the tight muscles in my body due to lack of sleep. Dedicated to the cause, I was progressing quickly—quicker than most—and by the end of the first month post-op, my morning yoga routine included standing poses.
I begged Mike daily for a chance to get on the bike.
That day finally came and I haven’t left the saddle since. I rode my first singletrack in Horseshoe Canyon with flat pedals at the end of May. And, today, I have more flexion in my bionic knee (about 140 to 145 degrees) than I ever did in my injured knee pre-op. My valgus leg deformity—that developed over years of compensation—is now gone. And, despite the six-inch scar down the center, my knee looks more like a real knee than it has in 20 years. While I still have a long way to go (they say full recovery takes one year), I consider myself a success story.
One Size Doesn’t Fit All
Not everyone is a candidate for knee replacement surgery, even if frequent discomfort is felt in the joint. Dr. Norene Christensen, PT, of Four Pines Physical Therapy in Jackson, urges younger people contemplating a total knee arthroplasty to keep their original parts as long as they can and to try cortisone injections or alternative healing modalities, like platelet-rich plasma therapy (PRP) or stem cell injections, first. She recommends having an internal conversation with yourself. “Be realistic and know that, at 60 or 65, you may need some sort of revision,” she says. “Manmade parts don’t last as long, and, fortunately, materials and surgical techniques will only improve over time.”
Dr. Lighthart agrees. “Consideration Number 1, 2, and 3 is the longevity of parts. The minute you put them in, you start the clock,” he says.
And Dr. Lee recommends trying everything else before getting a joint replacement, as it should be a last resort considered only when other measures have failed to provide relief, and only after educating yourself of the complications (while rare) that can happen after surgery, like blood clots or infection. Still, he applauds the merits of a good outcome.
People have a high level of activity [in our area]. They don’t want to slow down and they are not willing to sacrifice activity because they have a sore knee. So, if something can restore their level of activity, they go for it, even though there is some risk.”
— Dr. Kevin Lee, Upper Valley Orthopedics
“I’ve done replacements on people in their 60s, and they are coming back—now in their 80s—their [prosthetic] knee is still fine,” he adds, praising the new technology. “I think the 30-year knee is attainable, it’s not just a sales pitch. … Maintaining activity is so important that if your x-rays meet the need, there’s no question it’s the right thing to do.”
Check Yourself at the Door
If you tried everything and still wind up in the operating room—at St. John’s Hospital with Dr. Lighthart, Teton Valley Hospital with Dr. Mo Brown and Dr. Lee, or Madison Memorial Hospital, like I did, with Dr. Lee and a trusty robot—to receive a new knee, know it’s up to you to commit to and solidify your full recovery.
“It’s very important to have a good surgery that goes smoothly with no complications,” Bleffert says. “But your dedication to recovery—being committed and consistent, and doing the work at home—is crucial, especially during the first three months [post-op]. We usually train people past that because many of them want to go back to skiing and need a higher level of performance.”
Christensen acknowledges the importance of retraining your brain, too, after surgery. “Your brain is very pliable,” she says. “So, if you’ve been walking funny for five years because it’s ingrained in your motor patterns, you need to make sure your surgical knee isn’t just going along for the ride.”
My advice: Make sure this surgery is really what you want for yourself, as it’s no small feat. Then, find a doctor and physical therapist that specifically aligns with both your desired outcome and, equally important, your personality. It’s imperative to find skilled practitioners that you trust, especially if you want to continue to achieve a high level of activity. But, it’s also important to trust yourself, your instincts, and your ability to heal. Visualizing a pain-free and fully-functioning knee is the only way to get back to the sports you love—and with a whole new lease on life—whether you’re in your late 40s, like me, or well into your golden years.
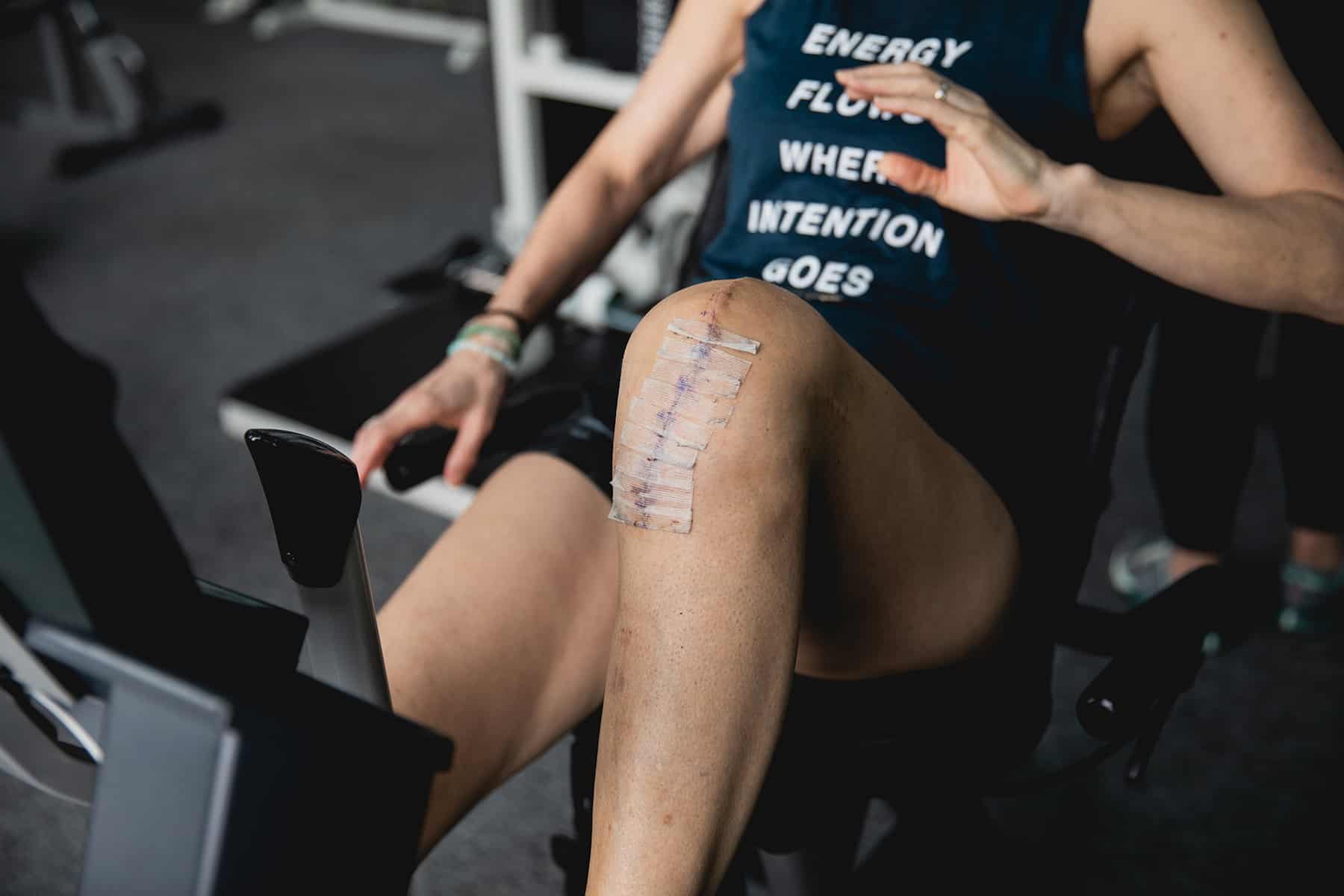
Firsthand knee replacement recovery advice (aka, what worked for me):
- Hit the gym and do yoga before surgery. (I attribute my speedy and full recovery more to my pre-surgery flexibility than to my muscle development and fitness level.)
- Make physical therapy your job. Do your exercises at home, even when it hurts, and use all my other recommendations to reduce the pain and swelling after.
- Eat an anti-inflammatory diet pre- and post-op. Or, at least cut out alcohol, wheat, dairy, and processed food.
- Integrate massage and acupuncturepre- and post-op. (Some doctors even prescribe this regimen.)
- Rent the fancy ice machine! I used the Nice 1 compression and ice machine (and, it doesn’t require ice!) available in Jackson from the MedCom Group.
- Get deep laser therapy treatments, available from Dr. Jim Davis or Dr. Eric Kunz in Driggs. (If it’s good for the NBA and the NFL, why not try it?)
- Take supplements, only after consulting your doctor. I took collagen, Vitamin D, Vitamin C, fermented cod liver oil (after discontinuing blood thinners), and proteolytic enzymes. My swelling was minimal.
- Stretch, even when you can’t really move.
- Bike your heart out, only after you get the clearance.